Often referred to as the “love drug” or “love hormone”, oxytocin has attracted increasing interest from researchers in recent years. It was originally shown to modulate aspects of social attachment and pair bonding in animals such as the female prairie vole, whose monogamous nature is dependent on oxytocin. Recent research in humans has shown that oxytocin increases trust behavior in economic exchanges and increases perception of trustworthiness in human faces, as well as promoting emotion recognition and altruism. This evidence inspired hopes among some, particularly in the mainstream media, that science might have found a possible pharmacological target for humans who show deficits in prosocial behavior.
But recent evidence has complicated the narrative a bit.
Research has shown that oxytocin plays a role in increased emotional reactivity to both positive and negative social cues. For example, one study from 2009 (Shamay-Tsoory et al) had participants engage in a game of chance with another player (the actor). In one condition, the actor was made to win more than the participant, evoking feelings of envy in the participant. In another condition, the actor was made to lose more than the participant, evoking feelings of “schaudenfrude” or gloating. Participants who were administered oxytocin before playing showed increases in both envy and schaudenfrude (if oxytocin was involved only in enhancing prosocial behavior, we would expect to see the opposite result.) Other research has shown oxytocin increased approach behavior or affiliative drive rather than regulating positive or negative responding per se. And one recent study showed that oxycotin led humans to self-sacrifice for their own group while showing increased aggression toward out-group members. The gist of this set of findings is that oxytocin doesn’t seem to bias individuals toward the positive, but rather can magnify whatever “stimuli” happens to be in someone’s attentional spotlight, be it bad or good, thereby generating an increase in corresponding positive or negative emotional responses.
Jennifer Bartz and colleagues (2010) were curious to explore whether oxytocin could “correct” deficits in pro-social behavior in individuals with borderline personality disorder (BPD), a population famous for emotional instability, extreme impulsive behavior and identity confusion. People with BPD tend to be involved in intense, emotionally volatile relationships characterized by frequent arguing, repeated breakups and extreme aggression. This behavior often extends beyond their romantic relationships, as BPD individuals have also been shown to have difficulty cooperating with strangers. The existing body of research, Bartz et al suggested, offers up contrary predictions. On the one hand, oxytocin could be helpful in reducing the negative behaviors normally associated with BPD in favor of kinder, gentler behavior towards others. Alternatively, oxytocin might have increasingly negative effects for people with BPD, who are chronically concerned with (lack of) trust and abandonment and have difficulty cooperating with others. They’re essentially fixed in a constitutively negative state when it comes to social interactions and increased oxytocin could decrease prosocial behavior even further. Additionally (or alternatively), the oxytocin system might be dysregulated in BPD and could produce different responses (vs. control) to oxytocin as a result.
Bartz and company designed an experiment in which the participant was paired with a partner (in reality, a virtual “computer” partner) to engage in an economic game. In this game, the participant was to make one of two choices that involved financial rewards. The catch was that the amount of the reward was also dependent upon the choice that their “partner” made.
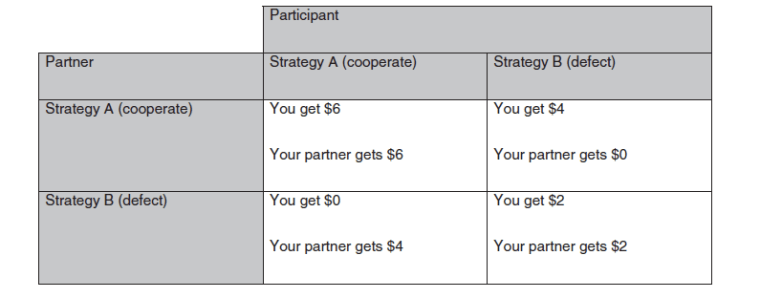
Both players clearly make the most money if they both choose strategy A. But because the player has to make the choice before the partner, the decision involves an element of trust (if your partner defects, you get nothing. If your partner trusts you and you defect, you get $4 and she gets nothing.)
So, what did they find?
Results showed the following:
1. BPD people trusted their partners in an economic game less after they received oxycotin than when they received a placebo.
2. Additionally, when asked if they would be more likely to make a hypothetical decision that would punish their partner, even when they knew their partner had extended trust toward them, they were more likely to punish after Oxytocin than placebo.
Administration of oxytocin to BPD individuals actually decreased pro-social behavior (and increased antisocial behavior). As the experimenters suggest, increasing the salience of a social cue that makes trust issues salient may have caused BPD participants to rely on their normal strategy for trust-dependent social interactions; that is, defect and punish the partner. Or it might have motivated approach/affiliative behaviors which triggered memory of past experiences gone awry and set off chronic and ever-present concerns about trust and rejection (e.g. “reject and punish them before they can do the same to me.”). Finally, the experimenters suggest the possibility that the oxytocin system itself may be dysregulated.
In short, the evidence doesn’t offer overwhelming support for the notion that exogenously-administered oxytocin will be a useful clinical treatment for people with pro-social deficits, such as those with BPD. Additionally, it’s difficult to imagine long-term benefits of oxytocin given that it’s half life when administered intranasally is only about three minutes. It’s been said that the most of the real action with regards to oxytocin is on the receptor end.
References:
Bartz, J., Simeon, D., Hamilton, H., Kim, S. Crystal, S., Braun, A., Vincens, V., & Hollander, E. Oxytocin can hinder trust and cooperation in borderline personality disorder. (2010). Social Cognitive & Affective Neuroscience
Shamay-Tsoory SG, Fischer M, Dvash J, Harari H, Perach-Bloom N, Levkovitz Y (November 2009). “Intranasal administration of oxytocin increases envy and schadenfreude (gloating)”. Biological Psychiatry 66 (9): 864–70.